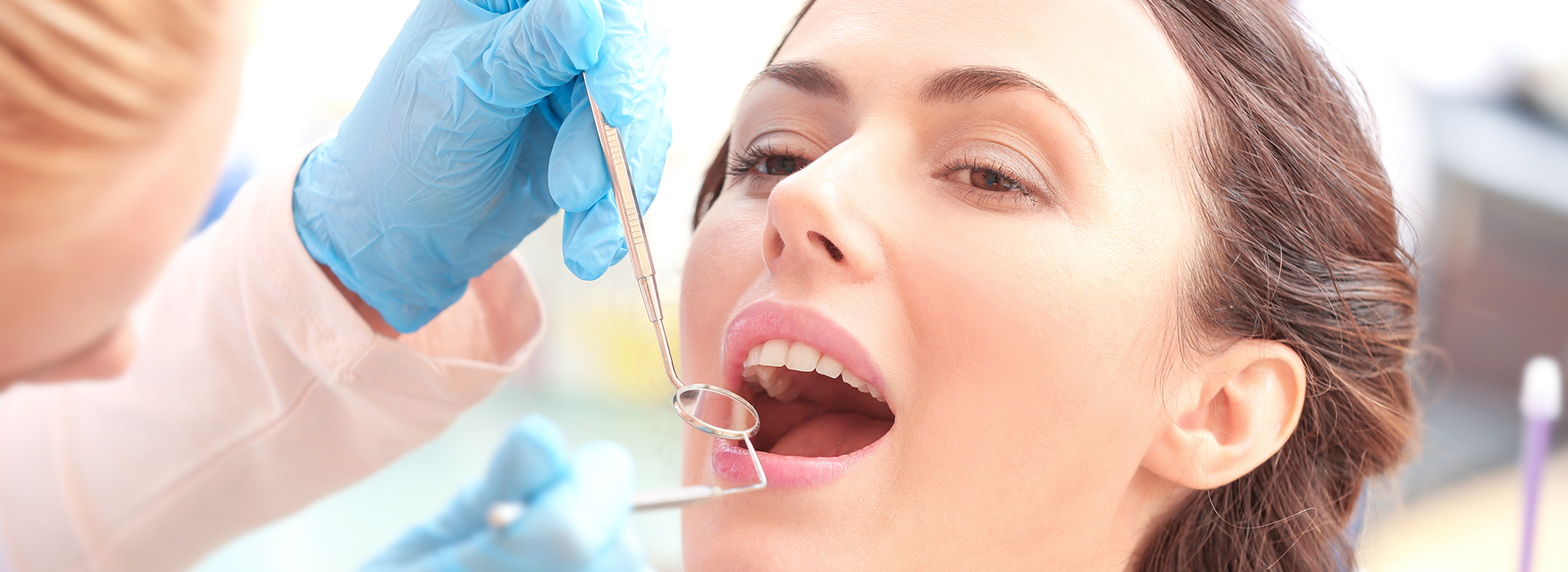
Gum disease is one of the most common—and most misunderstood—threats to an adult’s smile. Research shows that a large portion of adults develop some form of periodontal disease by middle age, yet many people don’t recognize the early signs. At the office of Whitesburg Dental Design, we focus on clear explanations, careful diagnosis, and practical treatment plans so patients can protect the tissues that hold their teeth in place.
Periodontal disease is an umbrella term for disorders that affect the periodontium—the gums, ligaments, and bone that support your teeth. It begins when bacterial plaque accumulates along the gumline and triggers an inflammatory response. Left unchecked, that inflammation damages the tissues that anchor teeth and can ultimately lead to tooth loss.
The process is usually gradual and often painless in the early stages, which is why many people only notice problems once damage has progressed. Routine exams and cleanings are the best way to catch changes early, before the condition advances to irreversible stages.
Being informed about how gum disease develops helps you make better choices every day. Effective home care, combined with professional maintenance, interrupts the cycle of plaque and inflammation and preserves both oral function and appearance.
Because gum disease can advance without obvious pain, spotting subtle changes is important. Early symptoms are often local—redness, puffiness, or bleeding when you brush—but they are meaningful signals that your gums are struggling with bacterial buildup and inflammation.
Other signs that warrant a prompt dental visit include gum recession, new gaps between teeth, persistent bad breath, or a change in how a bite feels. Addressing these signs early usually makes treatment less invasive and more predictable.
Some indications that you may have periodontal disease include:
Inflamed and red gums
Bleeding when brushing or flossing
Receding gums and exposed tooth root surfaces
Sensitivity to hot or cold temperatures
Bad breath or a bad taste in the mouth
Teeth that feel loose
New spaces developing between the teeth or a change in the bite
Change in the fit of existing partial dentures
Discharge around the teeth and gums
Sharp or dull pain when biting down or chewing food

Oral health does more than protect your smile—healthy gums play a role in overall wellness. Researchers have identified associations between periodontal inflammation and systemic conditions such as cardiovascular disease, diabetes control, and respiratory health. While links vary by individual, controlling gum inflammation is an important step toward better general health.
Prevention and early treatment matter because they reduce the inflammatory burden in the mouth and lower the risk that oral problems will complicate other medical conditions. Your dental team coordinates care with your broader health needs and tailors recommendations to your medical history.
With a focus on prevention, monitoring, and timely intervention, routine dental care becomes an essential component of long-term wellbeing—not just a way to keep teeth white.
Gingivitis is the initial, reversible stage of gum disease. It is characterized by inflammation without permanent tissue loss—red, tender gums and occasional bleeding are the most common signs. Because the damage at this stage is limited, treatment is usually straightforward and highly successful.
Addressing gingivitis means removing the causes of inflammation: plaque and tartar. Professional cleanings combined with an improved home-care routine typically resolve the condition. Patients who adopt consistent brushing, interdental cleaning, and regular dental visits can often avoid further progression.
Recognizing gingivitis early gives you the best chance of restoring healthy gum tissue without the need for surgical procedures. That’s why regular preventive care and honest conversations about daily habits are central to effective management.

If gingivitis remains untreated, it can progress to periodontitis—a stage where the inflammatory process damages the connective tissue and bone that support teeth. As pockets form around teeth, bacteria move deeper below the gumline and become harder to remove with routine brushing alone.
During periodontitis, patients may notice increased mobility of teeth, greater gum recession, and widening gaps between teeth. The primary goal of treatment at this stage is to stop further breakdown of supporting tissues and to restore a healthy environment around the teeth whenever possible.
Modern periodontal care offers several ways to address tissue loss and stabilize the mouth, from targeted debridement and medication to regenerative techniques that encourage bone and tissue repair when appropriate.
Effective periodontal therapy begins with a comprehensive assessment: measuring pocket depths, evaluating gum attachment and bone levels, and reviewing medical and lifestyle factors that influence healing. From that evaluation, a personalized plan is developed that prioritizes the least invasive, most effective options for each patient.
Treatment often follows a staged approach—starting with improved home care and professional deep cleanings, then using adjunctive therapies like localized antimicrobials or systemic medications if needed. When pockets are too deep or structural damage exists, surgical options are considered to restore form and function.
In addition to clinical procedures, long-term success depends on maintenance. Ongoing periodontal maintenance visits help monitor healing, control bacterial levels, and prevent recurrence so that results are durable over time.
When periodontal disease is caught early or tissue damage is limited, non-surgical treatments are the preferred starting point. Scaling and root planing—careful cleaning of root surfaces below the gumline—removes plaque and hardened tartar that fuel inflammation and pocketing.
These procedures are often paired with enhanced home-care instruction and may include the targeted use of antimicrobial agents placed beneath the gums or prescribed medications to reduce bacterial load. The objective is to reduce pocket depth, resolve inflammation, and make daily cleaning more effective.
Non-surgical approaches are both practical and evidence-based; when they succeed, patients avoid the need for more invasive interventions and enjoy predictable improvements in gum health.
When deeper pockets, significant bone loss, or other structural issues are present, periodontal surgery may be recommended. Surgical procedures can remove stubborn bacteria, reshape damaged tissues, and create a healthier architecture that patients can maintain. One common approach—flap surgery—exposes root surfaces and bone so they can be cleaned and repaired more thoroughly.
Surgeons may also use regenerative techniques, such as bone grafting and guided tissue regeneration, to encourage the body to rebuild lost structures. In select cases, lasers are used as adjuncts to reduce pocket depth and treat localized infection while minimizing soft-tissue trauma.
The goals of surgical periodontal therapy are specific: eliminate destructive bacteria, halt further bone loss, and recontour tissues to allow easier cleaning and long-term stability.
Remove sub-gingival bacteria beneath the gums and from the surfaces of the roots of the teeth
Halt damage to the underlying bone, and recontour the affected hard tissues as needed
Reduce pocket depth to facilitate easier cleaning of the teeth and gums and the maintenance of optimal periodontal health
With appropriate surgical care followed by disciplined maintenance and hygiene, many patients experience meaningful improvement in both comfort and function—even in cases that once seemed dire.
Your dental team will explain the rationale for any recommended procedure, the expected recovery, and the maintenance steps that will help sustain results over the long term.
We strive to provide clear, patient-centered periodontal care that preserves the tissues that matter most to your smile. If you would like to learn more about treatment options or schedule an evaluation, please contact us for more information.

Most people don’t realize that periodontal disease is the leading cause of tooth loss among adults. According to statistics from the Centers for Disease Control and Prevention, one out of every two adults over the age of 30 in the United States has periodontal disease.
You may be surprised to learn that the human mouth is home to a wide variety of microbes. The fact is that over 700 different strains of bacteria have been detected in the oral cavity. Although some of these bacteria are beneficial, others are harmful to oral health. Without proper oral hygiene and routine dental care, these harmful bacteria can cause tooth decay and gum disease, compromising both your oral health and overall wellbeing.
In addition to inadequate oral hygiene and infrequent professional care, other factors, including smoking, genetic tendencies, and unchecked diabetes, can contribute to the escalation of periodontal disease.
Your gums and teeth have an interdependent relationship, which means healthy teeth depend on the support of healthy gums. Also, taking care of your smile does more than keep your teeth and gums in optimal condition; good oral health also supports systemic health. In addition to being the leading cause of tooth loss in adults, researchers are finding more and more links between periodontal disease and a number of medical problems, including heart disease, stroke, diabetes, respiratory problems, and adverse pregnancy outcomes such as pre-term and low birth-weight babies.
If you notice that your gums are bleeding with the slightest pressure while brushing or flossing, it’s a sign of gingivitis. Although gingivitis is the earliest stage of gum disease, it can easily be reversed with deeper cleanings as well as an improved regimen of oral hygiene at home.
In the absence of professional treatment and better home care, gingivitis progresses to the next stage, which is known as periodontitis. In this stage, the connective tissue and bone that hold the teeth in place begin to break down with an increase in pocketing between the teeth and bone, gum recession, and bone loss. Without proper treatment by your dentist, periodontitis will progress from a mild to moderate loss of supporting tissue to the destruction of the bone around the teeth.
Although gingivitis can often be reversed with improved oral hygiene and professional cleanings, as periodontal disease advances, more extensive procedures are required to halt its progression. Based on a complete assessment of your periodontal health and a review of possible contributing factors, our office will recommend the best options in care. Treatment for periodontitis may include a series of deeper cleanings known as root planing and scaling, surgical procedures to reduce pocket depth, bone or tissue grafts, laser procedures, or antimicrobial medications.
The cost of care depends on the type of procedures required to restore your periodontal health. If you have dental insurance, plans often cover treatment to prevent gum disease as well as many procedures to treat the various stages of gum disease. Our goal is to help patients restore and maintain good oral health. We do all we can to help you begin care without additional stress or delay. Our business office works with you to maximize your benefits and provide easier, more convenient payment options.
By seeing our office regularly for care and doing your best to eat a healthy diet and practice good oral hygiene, you can keep your smile in tip-top shape as well as protect your overall wellbeing.
At the office of Whitesburg Dental Design, we provide a comprehensive range of services to address all your oral healthcare needs. You can rest assured that your smile is in the best of hands at our office. Our skilled and experienced team maintains a position at the forefront of advances in care and remains dedicated to providing the highest quality of skilled and compassionate treatment.
Periodontal disease begins when bacterial plaque builds up along the gumline and triggers an inflammatory response in the tissues that support teeth. Over time, plaque hardens into calculus (tartar) that harbors bacteria and makes daily cleaning less effective. If the inflammation continues unchecked, it can progress from reversible gingivitis to more destructive forms that affect bone and connective tissue.
Several factors influence how quickly gum disease develops, including smoking, uncontrolled diabetes, certain medications, hormonal changes, and genetic susceptibility. Poor oral hygiene and irregular professional care increase risk because they allow bacteria and inflammation to persist. Understanding these causes helps patients and clinicians target prevention and early intervention effectively.
Early signs of periodontal trouble often include red, tender, or swollen gums and bleeding during brushing or flossing. Many people also notice persistent bad breath, a bad taste in the mouth, or subtle gum recession that exposes more of the tooth surface. These symptoms can be mild at first and are easily overlooked, which is why awareness and routine exams are important.
If you observe any of these changes, schedule an evaluation rather than waiting for pain to develop, since pain frequently appears only after significant progression. Early detection typically allows for simpler, more predictable treatment and a better long-term outlook. Regular professional cleanings and at-home care are the most effective ways to catch and reverse early disease.
Diagnosis begins with a thorough clinical exam that includes measuring pocket depths around each tooth, checking gum attachment levels, and assessing bleeding and mobility. Dentists also review your medical history and may take dental radiographs to evaluate bone levels and hidden changes beneath the gums. This combination of probing, imaging, and health review provides a clear picture of disease stage and activity.
Accurate diagnosis informs a personalized treatment plan that targets the underlying bacterial infection and any contributing health factors. Periodic reassessment after initial therapy determines whether non-surgical care has been successful or if further intervention is needed. Clear communication about findings helps patients understand the reasons for recommended steps.
Non-surgical care is the first line of treatment for many patients and typically includes scaling and root planing to remove plaque and calculus from root surfaces beneath the gumline. These deep-cleaning procedures reduce bacterial load and allow inflamed tissue to heal, and they are often complemented by targeted antimicrobial therapy placed directly into periodontal pockets. Enhanced home-care instruction and correction of risk factors are integral parts of this approach.
When performed effectively, non-surgical therapy can reduce pocket depths, resolve inflammation, and stabilize the mouth without the need for surgery. Success depends on both the clinical procedure and the patient’s commitment to daily cleaning and follow-up visits. Your dental team will monitor response and recommend maintenance intervals to preserve improvement.
Surgical periodontal therapy is considered when deeper pockets, persistent infection, or significant bone loss prevent adequate cleaning and healing with non-surgical measures alone. Common surgical approaches include flap surgery to access and debride root surfaces, regenerative procedures such as bone grafting and guided tissue regeneration, and recontouring to restore a healthier architecture for maintenance. In some cases, lasers are used as adjuncts to reduce bacterial burden and improve soft-tissue management.
The primary goals of surgery are to eliminate destructive bacteria, halt further bone loss, and create conditions that make daily hygiene more effective. Recovery varies by procedure but generally involves short-term discomfort, careful post-operative hygiene, and follow-up visits to monitor healing. Your clinician will explain the rationale, expected outcomes, and aftercare steps so you can weigh benefits and plan for a smooth recovery.
Yes, appropriate periodontal treatment can often stabilize loose teeth and address bone loss when intervention occurs early enough to preserve supporting structures. Non-surgical therapy can reduce inflammation and improve attachment, while surgical regenerative techniques are designed to encourage bone and connective tissue repair in suitable cases. When structural support is severely compromised, stabilization methods such as splinting or restorative solutions may be used alongside periodontal care.
Not all teeth can be saved if damage is advanced; in those situations the focus shifts to preserving overall oral function and planning replacements that maintain health and chewing efficiency. Long-term success depends on the quality of the initial treatment and disciplined maintenance to prevent recurrence. Your dental team will discuss realistic expectations and a personalized plan based on the extent of disease.
Research has identified associations between periodontal inflammation and systemic conditions such as cardiovascular disease, diabetes control, adverse pregnancy outcomes, and respiratory health, though the nature and strength of these links vary among individuals. Chronic oral inflammation adds to the body’s overall inflammatory burden and can complicate management of other medical conditions. For patients with systemic health issues, controlling gum disease is an important part of a comprehensive wellness strategy.
Because oral and systemic health intersect, dental teams often coordinate care with physicians when relevant and consider medical history when planning periodontal therapy. Reducing oral inflammation through professional treatment and improved home care can support broader health goals and help minimize potential complications. Open communication about medications, medical conditions, and lifestyle factors improves treatment planning and outcomes.
Periodontal maintenance visits are more frequent and detailed than routine cleanings and focus on monitoring healing, controlling bacterial levels, and preventing recurrence of disease. These appointments typically include periodontal probing, targeted removal of subgingival deposits, reinforcement of home-care techniques, and periodic radiographs to check bone stability. Maintenance intervals are personalized and may range from every three months to longer based on individual risk and response.
Consistent maintenance is the cornerstone of long-term success because it allows early detection of changes and timely intervention before significant damage recurs. Patients who adhere to scheduled maintenance and recommended hygiene practices enjoy more predictable outcomes and a reduced need for additional invasive procedures. Your clinician will review results at each visit and adjust the plan as needed to sustain oral health.
Effective prevention combines thorough daily cleaning with regular professional care. Brush twice daily with a soft-bristled brush and fluoride toothpaste, clean between teeth once a day with floss or interdental brushes, and consider adjunctive measures such as antimicrobial rinses when recommended by your clinician. Lifestyle factors like quitting smoking and maintaining good blood sugar control for people with diabetes also play a major role in prevention.
Choosing the right tools and techniques for your mouth is best done in consultation with your dental team, who can demonstrate effective methods and tailor recommendations to your needs. Regular checkups and cleanings help remove buildup you can’t address at home and allow early intervention if changes occur. Prevention is both practical and highly effective when it becomes a consistent part of daily life.
The office of Whitesburg Dental Design in Huntsville evaluates periodontal health with a comprehensive, patient-centered process that blends careful assessment, evidence-based therapy, and clear education. Treatment plans prioritize the least invasive effective options, from scaling and root planing to regenerative or surgical procedures when appropriate, and they take medical history and risk factors into account. Technology and ongoing monitoring help clinicians measure progress and adapt care to each patient’s needs.
Education, prevention, and disciplined maintenance are emphasized to secure long-term results and protect overall wellness, and the team works with patients to build daily habits that support healing. By coordinating with other health providers when necessary and communicating expected outcomes, the practice aims to deliver periodontal care that preserves function, comfort, and a healthy smile. Patients are encouraged to schedule an evaluation if they notice symptoms or have risk factors for gum disease.

Ready to schedule your next dental appointment or have questions about our services?
Contacting Whitesburg Dental Design is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.