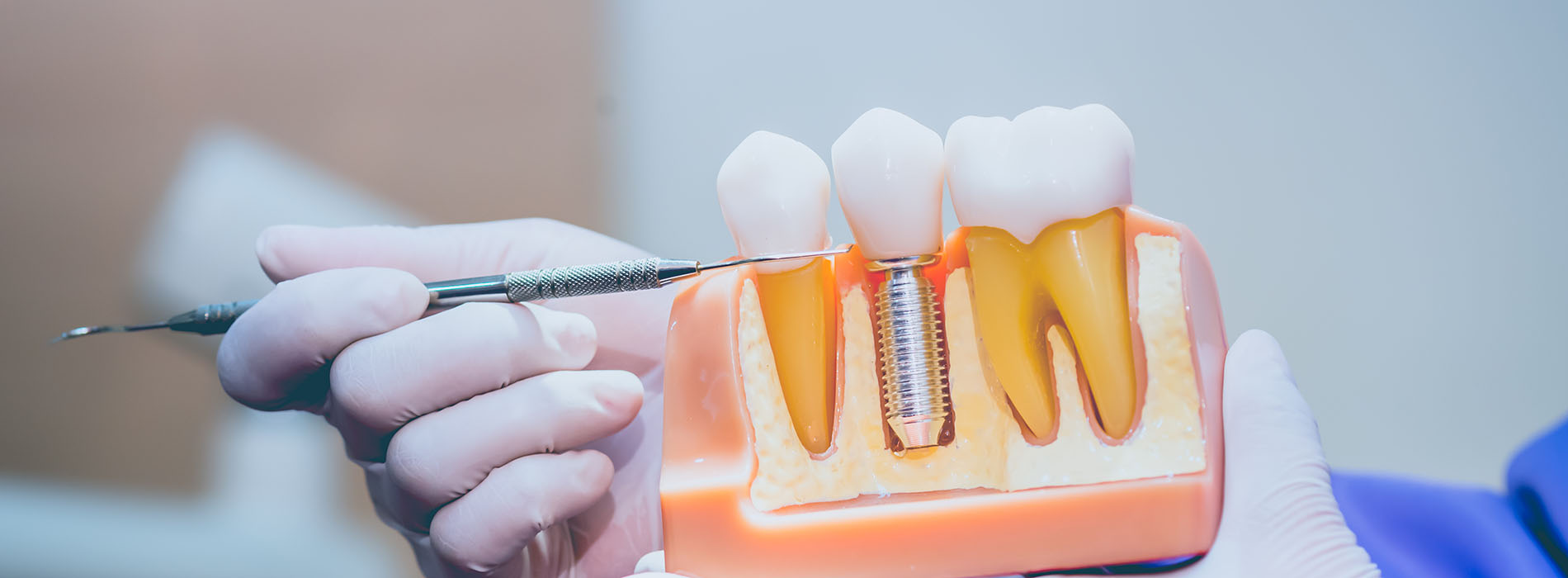
Implant restorations are the prosthetic crowns, bridges, or dentures that attach to dental implants to replace missing teeth. Unlike removable options that rest on the gums, implant restorations are anchored to titanium posts that bond with the jawbone, creating a stable foundation. This combination of engineered hardware and custom-crafted restorations aims to mimic the look, feel, and function of natural teeth, restoring both appearance and everyday oral performance for patients who have lost one or more teeth.
Technically, the implant itself functions as a substitute root, while the restoration is the visible portion designed to integrate with the surrounding teeth. Materials used for restorations—such as ceramic or porcelain fused to metal—are selected for strength and aesthetics, and they’re shaped to match each patient’s bite and smile. The restorative phase concentrates on precise fit, shade matching, and occlusion so the final result is comfortable, durable, and indistinguishable from adjacent natural teeth.
For many patients, understanding this distinction between implant and restoration helps set clear expectations: the implant provides structural support, and the restoration rebuilds the tooth’s form and function. Together they offer a long-term solution that addresses chewing stability, speech clarity, and facial support—helping prevent the gradual bone loss and shifting of neighboring teeth that often follow tooth loss.
After an implant has healed and integrated with the jawbone, the restorative process begins with careful planning. The clinician evaluates the implant’s position, surrounding gum tissue, and neighboring teeth to determine the most appropriate prosthetic design. Impressions or digital scans are taken to capture how the restoration should fit within the dental arch, and shade guides are used to achieve a natural color match. This planning stage lays the groundwork for a restoration that is comfortable, functional, and visually harmonious.
Next, a custom restoration is fabricated—either in a dental laboratory or with in-office digital milling equipment—based on those precise records. Temporary components may be used initially to shape the soft tissue or to provide function while the permanent piece is made. When the final restoration is ready, it will be carefully seated, adjusted for bite accuracy, and polished to blend with the adjacent teeth. The entire process emphasizes a stepwise approach to ensure predictable results and patient comfort.
Patients should expect follow-up visits to confirm fit and function after placement. During these check-ins, the dentist will verify that the restoration is performing as intended and that surrounding tissues remain healthy. Slight adjustments are common as the mouth adapts to the new restoration; these refinements help prevent uneven wear and ensure long-term comfort during chewing and speaking.
Implant restorations come in multiple forms to meet different needs. Single crowns replace an individual tooth and are ideal when one implant supports a solitary prosthetic. Implant-supported bridges span gaps where several adjacent teeth are missing—two or more implants can serve as anchors for a bridge, avoiding the need to alter neighboring natural teeth. For patients missing a full arch, implant-retained dentures or fixed full-arch restorations provide superior stability compared with conventional removable dentures.
Each type of restoration has design considerations that affect maintenance, hygiene, and long-term performance. For instance, a single crown allows easy access for flossing around an implant, while fixed full-arch restorations may incorporate specific cleaning aids or removable components to permit hygiene beneath the prosthesis. Your dental team will discuss which restorative format aligns best with your oral health status, lifestyle, and long-term goals.
Material choices also vary by restoration type. High-strength ceramics and porcelain deliver excellent aesthetics for single crowns, while hybrid or metal-reinforced frameworks may be recommended for larger span bridges or full-arch solutions where structural demands are greater. Careful selection ensures that the finished restoration balances beauty with the resilience required for daily function.
Implant restorations offer several important clinical advantages that go beyond filling a gap in the smile. Because implants transfer chewing forces to the jawbone in a manner similar to natural roots, they help preserve bone volume and facial contours that can otherwise deteriorate after tooth loss. Restorations attached to implants also prevent neighboring teeth from drifting into empty spaces, which reduces the risk of bite problems and uneven wear over time.
Functionally, implant-supported restorations provide greater bite strength and stability than traditional removable prosthetics, allowing patients to eat a wider variety of foods with confidence. They can also improve speech by restoring proper tooth positioning, which supports the lips and tongue during articulation. From an aesthetic perspective, modern restorative materials and techniques allow for highly natural-looking teeth that blend seamlessly with a patient’s existing dentition.
Patients who choose implant restorations often report a sense of normalcy and improved oral health because these solutions are designed for longevity and predictable performance. When planned and executed properly, implant restorations become a durable part of a comprehensive treatment strategy that supports both appearance and function for years to come.
Good oral hygiene is essential to protect both implants and their restorations. Daily brushing and flossing adapted to the type of restoration—using interdental brushes, floss threaders, or water irrigation when appropriate—helps remove plaque and reduce the risk of peri-implant inflammation. Professional cleanings and routine examinations allow your dental team to monitor tissue health, check the mechanical integrity of the restoration, and make timely adjustments if needed.
Regular monitoring is particularly important because complications, when they occur, are best managed early. Your dentist will inspect the implant-restoration interface, the surrounding gum tissue, and bite alignment at recall visits. Preventive care can help avoid common issues like screw loosening, minor wear, or soft tissue irritation, and it supports the long-term success of the restoration by addressing concerns before they escalate.
With appropriate home care and scheduled professional maintenance, implant restorations can remain functional and attractive for many years. Lifestyle choices that support oral health—such as avoiding tobacco and maintaining a balanced diet—also contribute to favorable outcomes. Your dental team will provide tailored recommendations to help protect your investment and maintain a healthy, confident smile.
Summary: Implant restorations combine advanced dental engineering with custom-crafted prosthetics to replace lost teeth in a way that restores appearance, function, and oral health. Whether you’re considering a single crown, an implant-supported bridge, or a full-arch solution, careful planning and ongoing maintenance are key to predictable, long-lasting results. If you’d like to learn more about implant restorations and how they might benefit your smile, please contact us for more information.

Implant restorations are the custom prosthetic crowns, bridges or dentures that attach to dental implants to replace missing teeth. These restorations are secured to titanium posts that bond with the jawbone, creating a stable foundation unlike removable prosthetics that rest on the gums. The combined system is designed to mimic the look, feel and function of natural teeth and to restore chewing, speech and facial support.
During planning, restorations are shaped and shaded to blend with adjacent teeth so the final result is comfortable and natural in appearance. Restorative materials and occlusal design are selected to balance aesthetics with long-term durability and wear resistance. A successful implant restoration recreates tooth form while protecting surrounding tissues and supporting overall oral health.
The dental implant is the titanium post that functions as a substitute tooth root and integrates with the jawbone, while the implant restoration is the visible prosthetic portion that replaces the crown of the tooth. The implant provides structural support and transfers chewing forces to bone, and the restoration restores form, color and function for everyday use. These two components work together but are distinct in purpose and design.
Between the implant and the restoration is an abutment or connector that secures the prosthesis to the implant and ensures proper fit and emergence profile. Proper planning of the implant position and the restorative design is essential so the final tooth aligns with the bite and surrounding gum tissue. Understanding this separation helps set realistic expectations for the treatment timeline and clinical steps involved.
Common implant restorations include single crowns for individual tooth replacement, implant-supported bridges for consecutive missing teeth and implant-retained or fixed full-arch restorations for patients missing most or all teeth. Implant-retained dentures may be removable for hygiene access, while fixed full-arch solutions provide a nonremovable restoration that functions like natural teeth. Each format addresses different functional and hygiene needs based on the number and position of missing teeth.
The design of the restoration influences maintenance, cleaning techniques and long-term performance, so your dental team will recommend the format that best fits your oral health and lifestyle. Smaller restorations like single crowns generally allow straightforward flossing around the implant, while larger frameworks may incorporate access points or specific hygiene tools. Material and connector choices are matched to the restoration type to ensure strength where needed and optimal aesthetics in the smile zone.
Implant restorations commonly use high-strength ceramics, zirconia, porcelain-fused-to-metal and hybrid frameworks depending on the clinical demands. Ceramics and zirconia are favored for their natural translucency and color-matching ability in visible areas, while reinforced frameworks or metal substructures can provide additional strength for long-span bridges or full-arch prostheses. Material selection balances esthetic goals with the mechanical demands of biting and chewing.
Your dentist will consider factors such as the restoration's location, opposing dentition, patient parafunction and esthetic expectations when choosing materials. Advances in digital milling and laboratory technology allow precision manufacturing that improves fit and reduces adjustments at delivery. The end goal is a restoration that looks natural, resists wear and integrates smoothly with surrounding teeth and tissues.
Once the implant has integrated with the jawbone, the restorative phase begins with a detailed clinical evaluation that includes checking tissue health, implant position and occlusion. Digital scans or impressions capture the exact tooth relationships and shade matching ensures the prosthetic will blend with your smile. The team at the office of Whitesburg Dental Design will plan the restoration to achieve proper fit, contour and function before fabrication.
Restorations may be fabricated in a dental laboratory or with in-office milling technology and temporary components can be used to shape soft tissue or provide function while the final piece is made. At delivery the restoration is seated, adjusted for bite accuracy and polished to harmonize with adjacent teeth, followed by short-term follow-up to confirm comfort and performance. Small refinements are common as the mouth adapts, and these adjustments help ensure predictable long-term results.
Daily oral hygiene is essential to protect implants and their restorations; brush twice a day with a soft-bristled brush and use interdental brushes, floss threaders or water irrigators to clean around the implant and under prosthetic components as appropriate. Removing plaque and food debris reduces the risk of peri-implant inflammation and helps preserve gum and bone health. Establishing a consistent home care routine supports long-term success and comfort with the restoration.
Avoiding tobacco and maintaining a balanced diet also contribute to favorable outcomes by supporting healing and tissue stability. Be attentive to any changes such as tenderness, swelling or looseness, and contact your dental team promptly if concerns arise. Regular professional cleanings complement home care by allowing early detection and management of potential issues.
Follow-up care typically includes scheduled recall visits for professional cleanings, inspection of soft tissues and assessment of the restoration's mechanical integrity. During these visits your dentist will check the implant-restoration interface, evaluate occlusion and confirm that surrounding tissues remain healthy. Early detection of minor problems such as screw loosening or soft tissue irritation makes corrective treatment simpler and more predictable.
Maintenance intervals are individualized based on oral health, prosthesis design and risk factors, but routine monitoring is essential to preserving results. Professional hygiene appointments may include use of specialized instruments and instructions for home-care adjustments tailored to the restoration type. Coordinated care between patient and clinician reduces complications and helps the restoration perform well for many years.
Good candidates for implant restorations are patients who are missing one or more teeth, have adequate jawbone volume or can undergo bone grafting when necessary, and demonstrate a commitment to regular oral hygiene and dental follow-up. A thorough medical and dental evaluation including imaging is used to confirm implant suitability and to identify any factors that could affect healing. Overall health, smoking status and certain systemic conditions are considered as part of the candidacy assessment.
Your dentist will review alternatives and recommend preoperative steps if needed, such as periodontal therapy or bone augmentation to create a stable foundation. When appropriate planning and preparation are completed, implants with well-designed restorations offer a durable and functional solution for many patients. The decision is based on individualized clinical findings and long-term oral health goals.
Common complications associated with implants and their restorations include peri-implant mucositis, peri-implantitis, screw loosening and minor wear or chipping of prosthetic materials. Peri-implant mucositis involves reversible inflammation of the soft tissues and is managed with improved hygiene and professional cleaning, while peri-implantitis may require more intensive non-surgical or surgical treatment depending on severity. Prosthetic issues such as screw loosening or wear are typically corrected by tightening, adjusting or replacing components to restore function.
Timely detection and prompt management are critical because early-stage problems are easier to treat and less likely to compromise implant stability. Regular checkups allow your dental team to monitor tissue health and prosthetic integrity and to recommend interventions when indicated. Patient adherence to home care and recall visits significantly reduces the risk of escalation and supports predictable outcomes.
You can schedule a consultation by calling (256) 539-9635 or by visiting our office at 2305 Whitesburg Drive, Huntsville, AL 35801 during regular business hours. During the initial consultation the dentist will review your medical and dental history, perform an oral exam and take any necessary imaging to evaluate bone volume and implant candidacy. This visit is focused on gathering information, answering questions and outlining appropriate restorative options tailored to your needs.
To prepare for the appointment bring a list of current medications and any recent dental records or X-rays if available, as this helps streamline diagnosis and planning. After the evaluation your dental team will explain recommended next steps, potential timelines and the clinical rationale for the chosen restoration type. Clear communication and coordinated planning ensure the proposed treatment aligns with your functional and esthetic goals.

Ready to schedule your next dental appointment or have questions about our services?
Contacting Whitesburg Dental Design is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.