Missing teeth change more than the way your smile looks — they affect how you chew, speak, and even how your face is supported. Modern implant dentistry is focused on restoring not only the appearance of a smile but the underlying function that lets people eat comfortably, speak clearly, and feel confident. Implants act as a durable foundation for replacement teeth and are engineered to work like the roots of natural teeth, which makes them a preferred long-term option for many patients.
Implants are a carefully planned treatment that begins with a thorough clinical evaluation. Using digital imaging and a detailed medical history, dentists can assess bone volume, soft-tissue quality, and overall health to design a personalized plan. When placed and restored well, implants provide stability that lets patients enjoy a broad diet and return to everyday life with minimal compromise.
At Whitesburg Dental Design, we combine contemporary technology with thoughtful patient education so people understand each step of the process. Our approach emphasizes predictable outcomes and practical solutions that align with a patient's needs, lifestyle, and oral health goals.

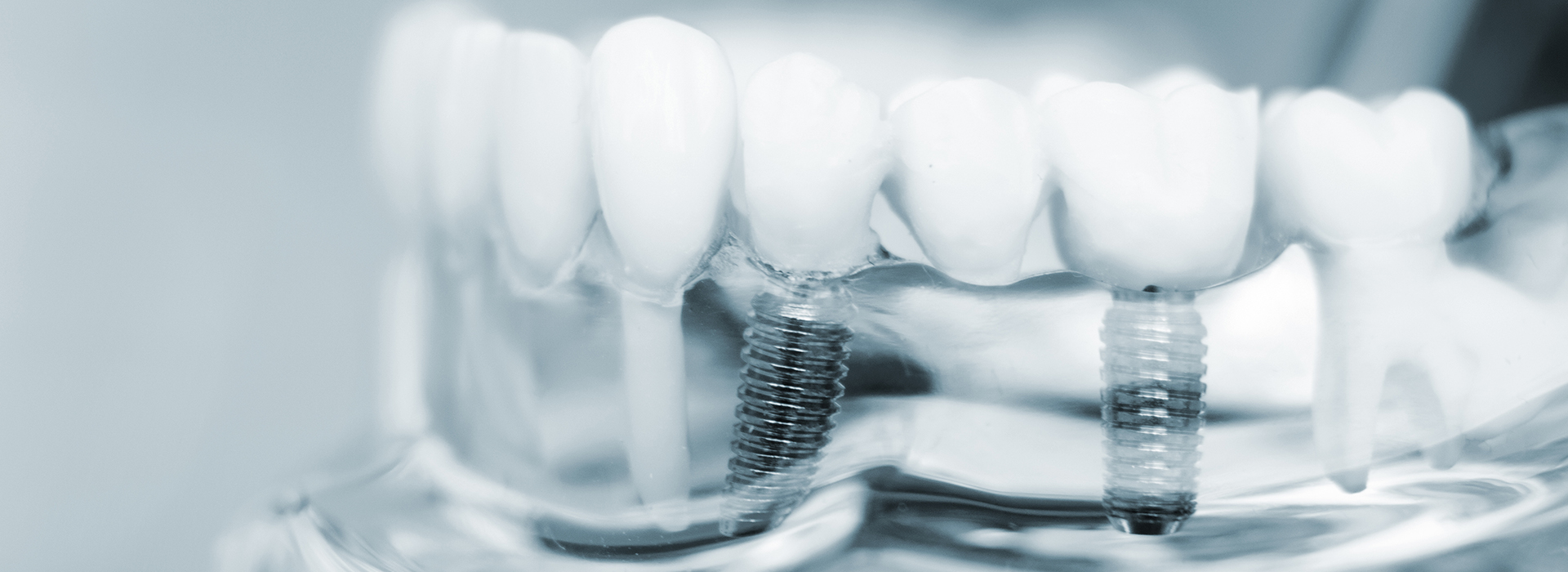
Dental implants are designed to mimic the entire tooth structure, not just the visible crown. A titanium or zirconia implant replaces the missing root, anchoring a crown, bridge, or denture so the replacement tooth behaves like a natural one. This root-like support preserves chewing efficiency, reduces movement of adjacent teeth, and helps maintain facial contours by providing stimulation to the underlying jawbone.
Because implants restore function at the root level, they eliminate many of the compromises associated with conventional removable dentures — speech is more natural, biting forces are better dispersed, and patients typically experience greater comfort. The materials used for implant-supported restorations are both durable and lifelike, so aesthetics and performance go hand in hand.
The key to implant success is osseointegration — the process in which bone gradually bonds to the implant surface. This biological fusion creates a stable platform for restorations and is why implants can reliably support single crowns as well as full-arch prostheses. The timeline to full integration varies based on the implant type, bone quality, and the specifics of the procedure, but careful planning helps set realistic expectations.
Advances in implant surface technology and imaging-guided placement have improved predictability and healing times. When planning implant therapy, clinicians evaluate bone density, proximity to anatomical structures, and the forces the restoration will need to withstand so the implant can be positioned for long-term success.
Implants deliver a range of practical benefits that directly affect daily life and oral health. Because they replace the root as well as the crown, implants support healthier bone levels and help maintain the natural architecture of the face. This preservation of bone prevents the sunken appearance that can follow long-term tooth loss.
In addition to bone preservation, implant-supported restorations avoid the need to alter neighboring healthy teeth when compared with traditional fixed bridges. They also reduce the risk of movement or slippage associated with removable dentures, giving patients more confidence when eating and speaking.

Implant dentistry is versatile: it can replace a single missing tooth, fill gaps caused by several missing teeth, or restore an entire arch. Each situation calls for a tailored plan that balances function, esthetics, and longevity. Whether the goal is a single crown that blends seamlessly with neighboring teeth or a full-arch solution that restores chewing capability, implants offer options for reliable, natural-looking results.
Treatment can be staged to match a patient's readiness and clinical needs. For some people, immediate provisional teeth can be placed while implants integrate; for others, a phased approach that allows for bone grafting and healing leads to the best long-term outcome. The right pathway depends on the clinical picture and the patient's goals.
Because no two smiles are exactly alike, successful treatment depends on detailed planning, precision in implant placement, and a well-crafted final restoration. Interdisciplinary coordination — including imaging, laboratory work, and restorative skill — is essential for predictable, comfortable results.
Good outcomes begin with careful preparation. A complete evaluation includes a medical and dental history review, a clinical exam, and diagnostic imaging such as CBCT scans when indicated. These steps reveal the quantity and quality of bone, the position of nerves and sinuses, and the relationship between upper and lower teeth — all of which guide precise implant placement.
Planning also includes reviewing habits and health factors that can influence healing, such as smoking, diabetes control, and certain medications. Where bone volume is insufficient, the treatment plan may incorporate grafting procedures to create a stable foundation for the implant.
Patient goals — from aesthetics to function and timing — are discussed up front so the team can design a plan that meets expectations while minimizing surprises during treatment.
Many adults who are in generally good health qualify for implants. The primary considerations are sufficient bone to support the implant, healthy gum tissue, and the ability to maintain oral hygiene. Age on its own is not a limiting factor; however, underlying medical conditions and lifestyle choices can affect candidacy and healing potential.
A dental implant consultation clarifies candidacy through physical examination and imaging. The clinician will explain which factors may require additional procedures, such as bone grafting or periodontal therapy, and outline a realistic timeline for treatment and recovery.
Implant placement is typically performed as an outpatient procedure. Many patients tolerate the surgery comfortably with local anesthesia, and sedative options are available for those who prefer additional relaxation. The complexity of the procedure varies: single implants may take only a short time to place, while full-arch treatments require more extensive planning and appointments.
After placement, a period of healing is needed for osseointegration. During this time, temporary restorations can often be provided to maintain aesthetics and function. Follow-up visits monitor healing and ensure the implant is integrating as expected. Once integration is confirmed, the definitive prosthesis — crown, bridge, or denture — is fabricated and attached.
Clear post-operative instructions and ongoing maintenance appointments are important to support long-term success. Patients are typically advised on gentle cleaning techniques, regular professional cleanings, and lifestyle habits that promote implant longevity.

Bone loss is a common consequence of tooth extraction, periodontal disease, or long-standing tooth loss. When there isn’t enough bone to safely place an implant, grafting can rebuild the site so an implant can be supported predictably. Grafts use a variety of materials — from the patient’s own bone to carefully selected graft substitutes — depending on the clinical situation.
Grafting procedures may be performed at the time of extraction, before implant placement, or simultaneously with implant surgery in selected cases. Healing times vary by graft type and the extent of augmentation, but modern grafting methods are highly successful and routinely used to create durable implant sites.
In areas where the upper jaw lacks vertical height near the sinus, a sinus lift can increase bone volume. Your clinician will explain any recommended grafting steps, the expected timeline, and how they fit into the overall implant plan.
Implant dentistry offers solutions that restore more than teeth — it restores daily function, confidence, and quality of life. By combining careful diagnostics, digital planning, and skilled restorative work, patients can achieve outcomes that feel natural and perform reliably for years.
Our team is committed to guiding patients through each stage of care with clear information and attentive follow-up so they can make informed decisions about their smiles. We focus on predictable, evidence-based approaches that prioritize long-term oral health.
If you’re considering implants or want to learn whether they’re the right option for your smile, please contact us for more information. We’ll review your situation, explain potential options, and help you take the next step toward a comfortable, complete smile.

If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.
Dental implants are titanium or zirconia posts surgically placed into the jaw to replace missing tooth roots. They provide a stable foundation for crowns, bridges, or dentures and are designed to mimic natural tooth function. Because implants integrate with bone, they restore chewing efficiency and help preserve facial contours.
The visible restoration, such as a crown, is attached to the implant by an abutment and is shaped to match surrounding teeth. Modern implant materials and prosthetic techniques focus on both function and a lifelike appearance. A thorough clinical and digital assessment guides material and design choices for each case.
Many adults are candidates for dental implants when they have adequate bone volume, healthy gum tissue, and systemic health that supports normal healing. Age alone is not a limiting factor, but conditions such as uncontrolled diabetes, heavy smoking, or certain medications can influence candidacy and timing. A comprehensive consultation with imaging and medical history review determines individualized eligibility.
When bone is insufficient, preparatory procedures like grafting or a sinus lift can create a stable site for implants. Periodontal health and oral hygiene habits are evaluated and often optimized before definitive treatment. Your clinician will outline alternatives and a realistic timeline based on the clinical findings.
Treatment planning begins with a detailed clinical exam and diagnostic imaging, commonly including CBCT scans to evaluate bone volume and anatomy. Digital impressions, occlusal analysis, and communication with the laboratory allow precise planning of implant position, angulation, and the final restoration. This interdisciplinary approach reduces surprises and improves predictability.
Surgical guides or computer-guided placement may be used to translate the plan into accurate intraoral results. Medical history review and preoperative instructions support safe anesthesia and healing. Clear communication about goals, timing, and follow-up care is an important part of the planning process.
Implant placement is typically an outpatient procedure performed under local anesthesia, with oral or IV sedation available for patients who prefer additional comfort. The implant is positioned into the prepared bone site and sutures are placed as needed to support healing. Single implants can often be completed in a relatively short appointment, while full-arch treatments may require staged surgical visits.
After surgery, an initial healing period allows osseointegration to occur, during which temporary restorations can maintain aesthetics and function when appropriate. Follow-up visits monitor healing and confirm readiness for the final prosthesis. The clinical team at Whitesburg Dental Design provides tailored post-operative instructions and schedules ongoing reviews.
Osseointegration is the biological process in which bone grows intimately against the implant surface, creating a stable bond that allows the implant to function like a natural tooth root. Successful osseointegration depends on factors such as bone quality, surgical technique, implant design, and patient health. The timeframe for integration varies but typically spans several weeks to a few months.
Advances in implant surface treatments and surgical protocols have improved the predictability and, in some cases, the speed of integration. Clinicians assess integration through clinical tests and imaging before placing the definitive restoration. Proper loading protocols and adherence to care instructions support long-term stability.
Bone grafting rebuilds lost jawbone to provide adequate support for implants and can use the patient’s own bone, donor bone, or synthetic substitutes depending on the situation. Grafting may be performed at the time of extraction, prior to implant placement, or simultaneously with implant surgery, based on the quality and quantity of available bone. Healing times vary with graft type and location, and the clinician will explain expected timelines.
A sinus lift is a specialized grafting technique used to increase vertical bone height in the upper jaw when the sinus floor is close to the proposed implant site. Careful imaging guides the decision to graft and determines the most appropriate technique. With modern materials and protocols, grafting procedures are routinely successful at creating stable implant sites.
Dental implants support a wide range of restorations, from single crowns that replace one tooth to implant-supported bridges and full-arch fixed prostheses that restore multiple missing teeth. Implant-retained overdentures provide a removable option that snaps onto implants for improved retention and easier hygiene. The choice of restoration balances functional needs, esthetic goals, and long-term maintenance considerations.
Fixed full-arch solutions commonly use four to six implants to create a non-removable restoration that mimics natural dentition, while partial solutions can replace specific missing teeth without altering adjacent healthy enamel. Laboratory communication and restorative design play a critical role in achieving proper occlusion, phonetics, and appearance. Your clinician will review restoration options and explain care requirements for each.
Immediate placement and provisionalization are possible in selected cases when primary stability is achieved and the clinical situation is favorable. This approach can preserve soft-tissue contours and reduce the overall treatment timeline for appropriately chosen patients. However, immediate loading is not suitable for every case, and clinicians evaluate risk factors such as bone quality and occlusal forces.
When immediate restoration is not indicated, a staged approach that allows undisturbed osseointegration often yields the most predictable long-term outcome. The treatment plan will clarify whether a temporary restoration will be used during healing and when the definitive prosthesis can be attached. Patient-specific factors determine the safest and most effective pathway.
Long-term success of implants depends on meticulous home care and regular professional maintenance to keep surrounding tissues healthy. Brushing twice daily, cleaning between teeth with floss or interdental brushes, and using nonabrasive toothpaste help control plaque around implants. Routine dental cleanings and periodic radiographs allow the clinical team to monitor bone levels and tissue health.
Avoiding tobacco and managing systemic conditions that affect healing support implant longevity. If signs such as redness, swelling, bleeding, or persistent discomfort occur, timely evaluation can identify early peri-implant disease and guide treatment. The team at Whitesburg Dental Design provides individualized maintenance schedules and practical hygiene instruction to help protect restored function and oral health.
Like any surgical procedure, implant therapy carries potential risks including infection, inadequate integration, nerve or sinus involvement, and peri-implant inflammation. Many complications are preventable with careful planning, sterile technique, and close post-operative follow-up. Early detection and intervention improve the likelihood of resolving issues without losing the implant.
Management options range from improved home care and nonsurgical therapy to surgical revision or removal in rare cases where the implant fails to integrate or disease persists. The clinician will discuss risk reduction strategies during your consultation and outline monitoring protocols to address complications promptly. Ongoing communication and adherence to follow-up visits are key to managing long-term risks.

Ready to schedule your next dental appointment or have questions about our services?
Contacting Whitesburg Dental Design is easy! Our friendly staff is available to assist you with scheduling appointments, answering inquiries about treatment options, and addressing any concerns you may have. Whether you prefer to give us a call, send us an email, or fill out our convenient online contact form, we're here to help. Don't wait to take the first step towards achieving the smile of your dreams – reach out to us today and discover the difference personalized dental care can make.